
1University School of Management Studies, GGS Indraprastha University, Dwarka, New Delhi, India
Creative Commons Non Commercial CC BY-NC: This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 License (http://www.creativecommons.org/licenses/by-nc/4.0/) which permits non-Commercial use, reproduction and distribution of the work without further permission provided the original work is attributed.
The 17 Sustainable Development Goals (SDGs) address the global challenges and aim to create a more sustainable and equitable world by 2030. As countries strive towards achieving these goals, SDG-3, which focuses on ensuring healthy lives and promoting well-being for all, is of paramount importance to build a sustainable health ecosystem. Countries must build a resilient health ecosystem which can sustain future pandemics as well. One of the prominent targets of this SDG is achieving Universal Health Coverage (UHC), which focuses on ensuring quality, accessibility, and affordability of health services for all. Digital health initiatives in the healthcare sector are one of the key emerging technologies and have gained enormous attention from healthcare organisations, various stakeholders, and even scholars. These technological interventions can further be leveraged to attain SDG-3. In light of these points, we conducted a hybrid-narrative review to provide a holistic view of the current literature, the opportunities, and the pitfalls for stakeholders. Further, future research directions for academicians were discussed. Digital health technologies can help in support of registration, financial support, the spread of awareness, unique identification, and maintenance of health records, which can facilitate a more robust healthcare system. A cascading model is presented for operationalising the role of digital health in achieving UHC and thus, moving towards a more sustainable healthcare system. Finally, the article summarises the key recommendations for various stakeholders and policymakers to maximise the impact of digital health for achieving UHC and thus, advancing the SDGs.
Health care management, technology & innovation, health information technology, management
Introduction
Digital health, or the integration of digital technologies in the healthcare domain, refers to the use of Information and Communications Technology (ICT) to support health and health-related fields (World Health Organization, 2019). With the integration of advanced hardware, software, and computing sciences, the term digital health is readily being used as an umbrella term encompassing numerous ICT initiatives in the healthcare industry (WHO, 2019). The concept of digital health technologies has been well-known for decades. Digital health includes numerous health system initiatives, including electronic health (eHealth), mobile health (mHealth), telemedicine, electronic medical records (EMR), wearable devices, remote monitoring, decision support systems, AI, robotics and many more.
However, since the COVID-19 pandemic, acceptance of digital health technologies has increased tremendously due to the health risks and lockdown restrictions imposed during the pandemic. The pandemic created a burden on healthcare delivery, and thus, across the world, digital technologies were integrated into the healthcare domain to tackle the disease threat associated with the sudden pandemic situation. These digital health tools have revolutionised the healthcare sector and transformed various aspects of the patient care delivery process.
With the adoption of modern technologies, the patient pathway can be more streamlined from symptom identification to treatment and further long-term support. With the potential of providing wider access to healthcare provisions, reduced costs, and patient-specific services, the healthcare industry has seen a paradigm shift post-pandemic (Awad et al., 2021). These technical capabilities are enabling new experiences for healthcare providers as well as for users. These new technologies can play a vital role in achieving health-related Sustainable Development Goals (SDGs) as well. The 17 SDGs were adopted by United Nations member states in 2015 and are considered an urgent call for action by all countries in a global partnership. Each nation is working towards these goals and is set to transform the world by 2030. These 17 goals comprise 169 targets, which cater to different aspects of sustainability.
For our study area, the SDG that is of foremost importance is SDG-3, which states ‘Ensure healthy lives and promote well-being for all at all ages’. This goal is related to the health and well-being of the population and comprises 13 targets that measure the progress and current state of healthcare facilities. This goal addresses all the major health priorities from reproductive to adolescent health, Universal Health Coverage (UHC), medicines and vaccines access, and many more.
UHC is one of the targets of SDG-3 and is considered a pivotal prerequisite to fight future pandemics. This target aims to provide healthcare services to a wider audience. UHC aims to provide quality healthcare services for all without any financial adversity (WHO) (Babatunde et al., 2021). UHC is an important target for SDG-3, and every nation is working towards achieving UHC and other SDG targets by the year 2030. With this target, along with the poor coverage and quality issues of care, the demand and supply aspect of health systems can also be addressed (Mehl et al., 2014). It is believed by the decision makers that UHC can act as a foundation for improving the population’s health, reaching a wider audience, achieving social justice, and also for economic progress. With comprehensive health governance and by minimising disparities, nations can also aim for resilient health systems through UHC (Id et al., 2022). Incorporating appropriate technologies in the form of eHealth and mHealth has the potential to increase health services coverage and impact.
Academicians in various fields, from medicine to management, have shown interest in this growing domain. However, the main focus is more on the user adoption perspective, and limited work around how these technologies can be leveraged for achieving UHC has been discussed. More importantly, there is a lack of a comprehensive view of the current state of digital technologies for UHC. The opportunities and pitfalls need to be addressed to understand how these digital initiatives can help in achieving UHC, which is one of the targets of SDG-3.
In this review, we contribute to the existing literature by mapping the gaps and opportunities to provide a holistic framework and the future research directions of this emerging technological intervention. Through our review, we answer the following research questions:
Our review emphasises scholars’ views on how digital health technologies can play a significant role in achieving UHC for SDG-3.
This article is organised as follows. The second section introduces the background literature, and the third section presents the literature search method. The fourth section outlines the synthesis of the literature. The fifth section outlines the key takeaways and future research directions. Finally, the sixth section presents our conclusion.
Background Literature
The healthcare sector is revamping to incorporate digital health technologies and is moving towards a massive digital transformation these days (Gleiss & Lewandowski, 2022). This digital transformation is enabling the healthcare sector to move from the ongoing ‘one-size-fits-all’ approach to a more patient-centric approach. These digital health solutions are capable of improving the prognosis and diagnosis of diseases, as well as enhancing the whole care delivery process. With digital technology and remote monitoring in place, patients can monitor their health regularly and have better control of their health and health-related decisions (Awad et al., 2021). Digital health is used as an umbrella term for numerous health system initiatives, including eHealth, mobile health (mHealth), telemedicine, EMR, wearable devices, remote monitoring, decision support systems, AI, robotics, and many more. These technological initiatives offer a plethora of growth opportunities for the healthcare domain. They can enhance healthcare access, provide better integration of data from different sources, improve provider-patient communication, provision of electronic decision support, and thus, strengthen the healthcare sector and delivery process across the world.
These digital solutions can help in bridging the gap between the service provider and the patients. With the onset of the pandemic in 2020, healthcare delivery across the globe has been adversely affected. In India, with limited medical assistance and limited health infrastructure, people were forced to use digital technologies to consult a healthcare provider and had to opt for remote monitoring via mHealth and teleconsultation. As per a survey, COVID-19 removed several digital transformation barriers in the healthcare sector when compared to the pre-pandemic era. According to their survey, 51% of healthcare providers and organisations increased their usage of digital technologies during the pandemic to connect with patients and the public. 75% of people reported that digital solutions enhanced the healthcare delivery process both for the patients and service providers, and around 78% of Indian respondents felt that digital solutions help them access healthcare when and where needed. There was a remarkable three times increase in the number of people opting for online consultation. Though the statistics of online healthcare users increased, many healthcare organisations continually face the issue of maintaining access to care, providing services operating within a budget, and also managing the workforce capacity; thus, the need for the right digital tools and integration with medical needs is still a concern for many.
Thus, there is a need for healthcare organisations to evaluate how these digital health technologies can be leveraged to strengthen the care delivery process for the future. Post-pandemic, these health technologies are being readily accepted by healthcare providers and patients to connect, monitor, and improve health. These technologies can further be leveraged to achieve the SDGs by the nation. With the accessibility, affordability, and interoperability features of digital health, this technology can act as a facilitator to achieve the SDGs by 2030.
The COVID-19 pandemic exacerbated the healthcare burden manifold and thus, resulted in infecting more than 500 million people by mid-2022, and led to 15 million deaths by 2021. This pandemic disrupted the essential healthcare services in 92% of countries across the world and thus halted the global UHC process. As the global life expectancy and immunisation coverage rate fell during this period, the prevalence of anxiety and depression amongst the population amplified (UN, n.d.).
eHealth is considered the cost-effective and secure use of ICT for supporting health and health-related fields. Whereas, mHealth refers to the use of mobile or wireless technology for health (WHO, 2016). It is believed that through the accessibility and interoperability features of digital health, nations can move from disease-centric silos to resilient healthcare systems, which can help in facilitating UHC at a faster rate (WHO, 2016). Thus, it will be crucial to understand what are the opportunities and pitfalls of using digital health for achieving UHC and SDG-3 by nations.
Literature Search Method
We conducted a hybrid-narrative review, for which the selected studies were integrated and a framework was designed. Further, the future research directions were drawn using a narrative style (Dincelli & Yayla, 2022; Paul & Criado, 2020). To limit the scope of our literature, we included articles published after 2017. First, we searched for keywords UHC, digital health and related keywords in the Title, Abstract, and Keywords categories in Scopus and Web of Science. This initial search yielded 608 results. Next, we further excluded studies that were not in the English language and those which were not journal articles. We considered only those articles which were in the management, health literacy, and social sciences domains. The articles which were extracted were further filtered based on the year of publication, as we only considered literature from 2015 to 2023. The final 474 results were further screened based on Title, Abstract, and Keywords. This systematic search resulted in 27 articles on UHC using technological initiatives. Figure 1 shows our search strategy (Figure 1). The Boolean string was as follows:
Figure 1. PRISMA Flow Diagram for the Articles’ Selection Process.
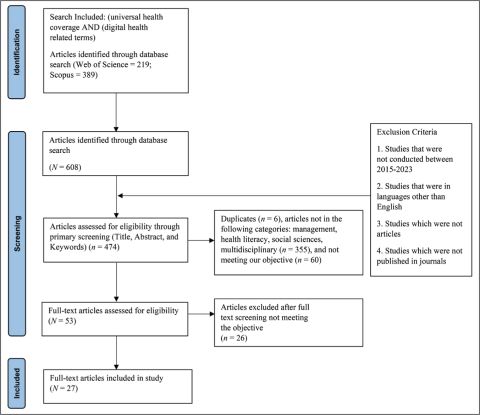
Results
In this section, we present our results in answers to RQs and provide an analysis of the studies in our research. Our analysis started by determining the descriptive statistics of the 27 research articles in our database, in terms of region-wise distribution, study approach, and year of publication, to understand the literature trends. Various articles published between 2015 and 2023 follow a consistently increasing trend, from seven articles between 2016 and 2019 to 20 articles between 2020 and 2023, which points towards the growing interest in this research field. Despite the growing academic interest, there is still scope for new developments for determining how digital health technologies can be leveraged for UHC achievement by nations (Table 1).
Table 1. Articles Distribution by World Health Organization Region, Study Approach, and Year (N = 27).
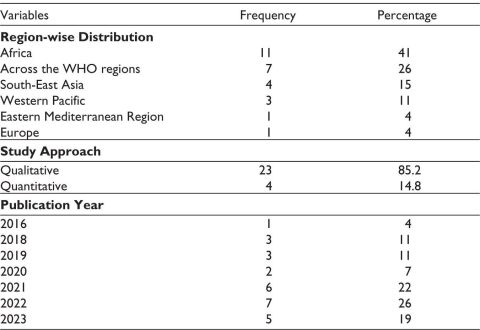
The approach or methodology used by around 85% of the studies is a qualitative approach, and only one article used a mixed-method approach. Around 41% of articles were from the WHO Africa region, and another 26% were across two or more WHO regions.
An overview of the articles included in our study is presented in Table 2 to better understand the objective and main findings of the study (Table 2).
Table 2. Opportunities and Pitfalls of Achieving UHC Through Digital Health.

We can answer our first RQ by analysing the current literature. Our first RQ focuses on the current state of literature about UHC through a digital health perspective. Through the literature in our study, we can see that the majority of authors are discussing the need to achieve UHC for SDG attainment by 2030. However, limited scholarly work on framework formation has been done. The current literature focuses more on the opportunities and pitfalls of achieving UHC and how digital health can help in attaining this SDG target. The current literature also emphasises the need for region-specific policies for the attainment of UHC, as a ‘one-size-fits-all’ approach cannot formulate generalised techniques for achieving UHC. UHC is one of the major targets of SDG-3; hence, nations need to involve more stakeholders and create effective policies to attain UHC. Academicians strongly believe that digital health technologies can tackle many challenges of access coverage, like financial constraints, geographic connectivity, reaching a wider audience, providing quality healthcare, and also easy accessibility and interoperability.
Our RQ focuses on the opportunities and pitfalls for achieving UHC through digital health technologies. The major pitfalls for using digital health technologies for UHC involve internet connectivity issues, mobile ownership issues, ineffective policies, lack of awareness, and limited regulation of digital health. The opportunities of digital health can help in providing healthcare access to a wider region, which can be accessible at any time, affordable, and can reduce financial constraints. With the interoperability feature of digital health, the government can form a centralised platform for easy integration of healthcare data from various sources. Digital health technology can also help enhance the healthcare delivery service process and also, and can provide real-time reports, remote monitoring, and follow-up messages. Medical records can also be stored online and retrieved anytime when needed. We have presented (Table 2) the inferred opportunities and pitfalls.
Thus, we can say digital health technologies are capable of transforming the healthcare system and helping in achieving UHC and thus, SDG-3.
Our third research question focuses on future research direction. Despite the growing literature on the usage of digital health technology for the healthcare industry, academicians are mainly studying the intention or adoption factors that can enable or inhibit the growth of digitisation in the healthcare domain. As nations are moving towards a more sustainable world and working towards achieving the goals formulated by the UN, researchers can focus more on developing frameworks for achieving UHC and other targets of SDG-3 using digital health technologies. The integration perspective of digital health with the healthcare ecosystem is still missing and needs to be addressed for the attainment of SDGs.
Discussion
However, there has been extensive work on why UHC is relevant for the nations or how digital health can support the growth of SDGs and UHC achievement, particularly. Despite the potential of digital health for UHC achievement, our review suggests that for the achievement of UHC, the adoption and coverage process comes with challenges. In Figure 2, we bring together how digital health technologies can be utilised for the achievement of UHC. To create our framework, we adapted the Tanahashi model (Tanahashi, 1978) which evaluates health coverage needs and helps in identifying bottlenecks in the operation process. This framework (Figure 2) is adapted from (Mehl et al., 2014) and (WHO, 2019) and aims to provide suggestions and strategies for the integration of digital health technologies for UHC.
Figure 2. Cascading Model for Integrating Digital Health with UHC.
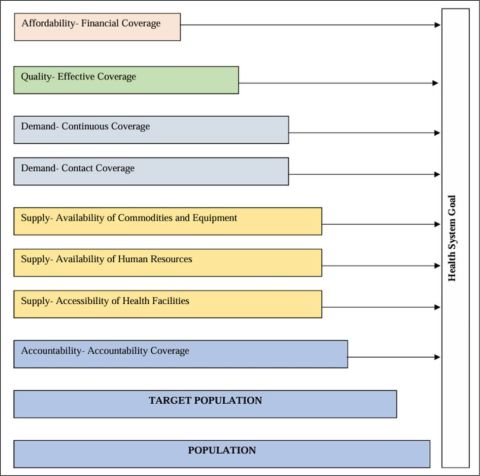
The cascading model, which is used for studying health coverage needs help in assessing the bottlenecks and thus, formulating future strategies. There are various goals of health services, which are represented as different layers of Tanahashi’s cascading model. For our framework, we would like to suggest strategies for all these health services layers to achieve UHC through digital health. We would like to suggest the following strategies for achieving health services goals:
Thus, these layers provide potential challenges that nations can face while achieving UHC, and our strategies also provide some digital health integration opportunities for leveraging UHC and achieving SDG-3.
Conclusion
Digital health technologies are advancing rapidly as more powerful, interoperable, and accessible tools are set to transform the healthcare ecosystem. These technologies can be utilised for achieving SDG-3, which focuses on the good health and well-being of all. Realising this rapid growth and interest, we provided a synthesis of literature focusing on the UHC target of SDG-3, through the integration of digital health technologies. Current technological advancements can accelerate the process of UHC and help nations in providing accessible, affordable, and quality health services to all. Based on the Tanahashi framework health services goal, we have also provided strategies for achieving universal health access using technology integration. With the consideration of major opportunities and pitfalls, stakeholders and policymakers could benefit from this emerging technology field.
Our review also showed that scholarly work around the relevance of UHC achievement has been conducted. The need for digital health technologies for UHC is also readily discussed by the authors. As UHC is an integral part of SDG-3, it can help in building a resilient framework for future pandemics and health issues. Thus, leveraging digital health technologies can help in creating a sustainable healthcare ecosystem and improve the health infrastructure for future pandemics.
Implications
This study has the following implications. First, Policymakers should strengthen their privacy and security framework to safeguard the health-related data. Second, investments in digital infrastructure can help in facilitating robust mechanisms for storing health-related information like EHRs and also for predictive analysis for future pandemics and epidemics. Third, Healthcare providers can use these digital technologies to enhance patient care, upskill their staff, and facilitate better remote monitoring options for their patients by leveraging telehealth and telemedicine. Future researchers can investigate the intersection of public health and digital health to expand theoretical frameworks.
Authors’ Contribution
Both authors contributed equally to this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
ORCID iDs
Anushka Goel  https://orcid.org/0000-0003-3507-8169
https://orcid.org/0000-0003-3507-8169
Udita Taneja  https://orcid.org/0000-0002-4494-4244
https://orcid.org/0000-0002-4494-4244
Awad, A., Trenfield, S. J., Pollard, T. D., Ong, J. J., McCoubrey, L. E., Goyanes, A., Gaisford, S., & Abdul, W. (2021). Connected healthcare: Improving patient care using digital health. Advanced Drug Delivery Reviews, 113958. https://doi.org/10.1016/j.addr.2021.113958
Babatunde, A. O., Abdulkareem, A. A., Akinwande, F. O., Adebayo, A. O., Omenogor, E. T., Adebisi, Y. A., & Ilesanmi, E. B. (2021). Leveraging mobile health technology towards achieving universal health coverage in Nigeria. Public Health in Practice, 2, 100120. https://doi.org/10.1016/j.puhip.2021.100120
Dincelli, E., & Yayla, A. (2022). Immersive virtual reality in the age of the Metaverse: A hybrid-narrative review based on the technology affordance perspective. Journal of Strategic Information Systems, 31(2), 101717. https://doi.org/10.1016/j.jsis.2022.101717
Gleiss, A., & Lewandowski, S. (2022). Removing barriers for digital health through organizing ambidexterity in hospitals. Journal of Public Health (Germany), 30(1), 21–35. https://doi.org/10.1007/s10389-021-01532-y
Id, A. E., Gilks, C. F., Ambaw, F., & Assefa, Y. (2022). Universality of universal health coverage: A scoping review. 1–15. https://doi.org/10.1371/journal.pone.0269507
Mehl, G., Labrique, A., & District, U. (2014). Prioritizing integrated mHealth strategies for universal health coverage. Global Health Action, 345, 6202.
Paul, J., & Criado, A. R. (2020). The art of writing literature review: What do we know and what do we need to know? International Business Review, 29(4), 101717. https://doi.org/10.1016/j.ibusrev.2020.101717
Tanahashi, T. (1978). Health service coverage and its evaluation. Bulletin of the World Health Organization, 56(2), 295–303.
World Health Organization. (2019). Recommendations on digital interventions for health system strengthening: Evidence and recommendations. https://www.who.int/publications/i/item/9789241550505